Today in this article we will discuss about What is Hepatitis PDF and PPT Download, A Complete Guide to Types, Symptoms, Causes, Diagnosis, and Treatment so, Hepatitis is one of the most common and serious liver conditions affecting millions of people around the world. Whether you just heard the word for the first time or you are trying to understand a recent lab result like hepatitis B surface antigen reactive or hepatitis B surface antibody positive, this guide will walk you through everything you need to know in clear, simple language. In this article blog, we cover what hepatitis is, what causes it, the different types including hepatitis A, B, C, D, and E, the symptoms to watch for, how it is diagnosed, whether it is curable, and the treatment options available today including medications like Harvoni, Epclusa, Mavyret, and Bulevirtide.
What is Hepatitis? Understanding the Basics
Hepatitis is inflammation of the liver. The liver is a vital organ that filters your blood, helps digest food, and removes toxins from the body. When the liver becomes inflamed or damaged, it cannot perform these functions properly.
The word ‘hepatitis’ comes from the Greek word ‘hepar’ meaning liver, and ‘itis’ meaning inflammation. Hepatitis is a hepatitis disease that can be short-term (acute) or long-term (chronic), depending on the cause and how the body responds.
Chronic hepatitis is a term used when liver inflammation persists for more than six months. This long-term form of the disease is particularly dangerous because it can silently damage the liver over years, potentially leading to cirrhosis, liver failure, or even liver cancer.
What is Hepatitis PDF and PPT Download (.PPTX) – 105 PPT SILDES
What Causes Hepatitis? The Most Common Reasons
So what causes hepatitis? The causes of hepatitis fall into several broad categories. Knowing the cause is the first step to getting the right treatment.
1. Viral Infections
The most common cause of hepatitis worldwide is infection by hepatitis viruses. There are five main types of hepatitis viruses, each with unique characteristics:
- Hepatitis A Virus (HAV)
- Hepatitis B Virus (HBV)
- Hepatitis C Virus (HCV)
- Hepatitis D Virus (HDV) also known as the D virus
- Hepatitis E Virus (HEV)
2. Heavy Alcohol Use
Drinking large amounts of alcohol over a long period damages liver cells and causes alcoholic hepatitis. This form is not contagious but can be just as serious.
3. Autoimmune Disorders
In autoimmune hepatitis, the immune system mistakenly attacks liver cells, treating them as foreign invaders. This is not caused by a virus and is not a communicable disease.
4. Drugs and Toxins
Certain medications, herbal supplements, and chemicals can cause liver inflammation. This is called drug-induced hepatitis.
5. Non-Alcoholic Fatty Liver Disease (NAFLD)
Fat accumulation in the liver, not caused by alcohol, can also lead to hepatitis-like inflammation.
Is Hepatitis a Communicable Disease?
This is a very common question. Is hepatitis a communicable disease? The answer depends on the type. Viral hepatitis types A, B, C, D, and E are all communicable diseases, meaning they can spread from person to person. However, alcoholic hepatitis and autoimmune hepatitis are not contagious.
Understanding whether hepatitis is contagious depends heavily on the specific virus involved and the route of transmission.
Types of Hepatitis: What is Hepatitis A, B, C, D, and E?
What is Hepatitis A?
Hepatitis A is a short-term, acute liver infection caused by the hepatitis A virus (HAV). It does not usually become a chronic condition, and most people fully recover.
Hepatitis A is mainly spread through contaminated food or water, especially in regions with poor sanitation. It is highly contagious. Symptoms usually appear 2 to 6 weeks after exposure and include fatigue, nausea, jaundice (yellowing of the skin and eyes), abdominal pain, and dark urine.
A safe and effective vaccine is available to prevent hepatitis A.
What is Hepatitis B?
Hepatitis B is a serious liver infection caused by the hepatitis B virus (HBV). It can be both acute and chronic. Hepatitis B is transmitted by contact with infectious body fluids including blood, semen, and vaginal fluids.
Hepatitis B is transmitted by:
- Unprotected sexual contact with an infected person
- Sharing needles or syringes
- Mother to baby during childbirth
- Sharing personal items like razors or toothbrushes with an infected person
- Needlestick injuries in healthcare settings
Hepatitis B is preventable with a vaccine. Globally, over 296 million people live with chronic hepatitis B.
Understanding Hepatitis B Lab Results
If you have had blood tests recently, you may have come across terms that are confusing. Here is a breakdown of common hepatitis B test results and what they mean:
Hepatitis B Surface Antigen (HBsAg)
The hepatitis B surface antigen is a protein found on the surface of the hepatitis B virus. It is the earliest indicator of a current hepatitis B infection.
- Hepatitis B surface antigen reactive or hepatitis B surface antigen positive: This means the virus is present in your blood. You currently have a hepatitis B infection and can spread it to others.
- Hepatitis B surface antigen non reactive or hepatitis B surface antigen negative: The virus is not detected. You are not currently infected with hepatitis B.
Hepatitis B Surface Antibody (HBsAb / Anti-HBs)
The hepatitis B surface antibody, also written as hepatitis B surface ab, is produced by your immune system in response to the hepatitis B virus or vaccination. It indicates protection or immunity.
- Hepatitis B surface antibody reactive or hepatitis B surface antibody positive: You have developed antibodies to hepatitis B. This means you are immune, either from vaccination or recovery from a past infection.
- Hepatitis B surface ab reactive: Same as above. Your body is protected from future infection.
- Hepatitis B antibody reactive or hepatitis B antibody positive: Similar meaning. Your immune system has responded to the virus.
Hepatitis B Surface Antigen vs. Antibody: What is the Difference?
An antigen is part of the virus itself. An antibody is what your immune system produces to fight the virus. If you are hepatitis B surface antigen reactive, you are infected. If you are hepatitis B surface antibody reactive, you are protected.
Hepatitis B Reactive vs. Non Reactive
When your doctor says you are hepatitis B reactive, it typically means one of your hepatitis B markers has come back positive and needs further evaluation. Hepatitis B non reactive means no current infection or immunity markers are detected. Your doctor will interpret these results in the context of your full panel.
What is Hepatitis C?
Hepatitis C is a viral infection that causes liver inflammation and is transmitted primarily through blood-to-blood contact. It is the most common blood-borne viral infection in many countries.
Unlike hepatitis A and B, there is no vaccine for hepatitis C. However, it is highly curable with modern medications. About 80 percent of people infected with hepatitis C will develop chronic infection if left untreated.
Hepatitis C is mainly spread through sharing needles, syringes, or other drug-using equipment, and through blood transfusions with unscreened blood. Sexual transmission is possible but less common.
What is Hepatitis D?
Hepatitis D, sometimes called the D virus or delta hepatitis, is a liver infection caused by the hepatitis D virus (HDV). This virus is unique because it can only infect people who already have a hepatitis B infection. It cannot survive on its own.
Hepatitis D can occur as a co-infection with hepatitis B or as a superinfection in someone with chronic hepatitis B. Superinfection often leads to more severe disease and faster liver damage.
Hepatitis D treatment has historically been limited, but newer medications have changed that. The drug bulevirtide has been approved in Europe and is showing strong results for hepatitis D treatments. Bulevirtide works by blocking the virus from entering liver cells. Pegylated interferon alfa has also been used for hepatitis D treatment for many years. Discuss hepatitis D treatments with a specialist hepatologist for the most current guidance.
What is Hepatitis E?
Hepatitis E is caused by the hepatitis E virus (HEV). It is most common in South Asia, East Asia, and parts of Africa and the Middle East. It is primarily spread through contaminated drinking water.
For most people, hepatitis E is a self-limiting disease that resolves on its own within 4 to 6 weeks. However, it can be very dangerous for pregnant women, especially in the third trimester, where it can cause acute liver failure and a high mortality rate.
There is a vaccine available in China but not yet widely approved elsewhere.
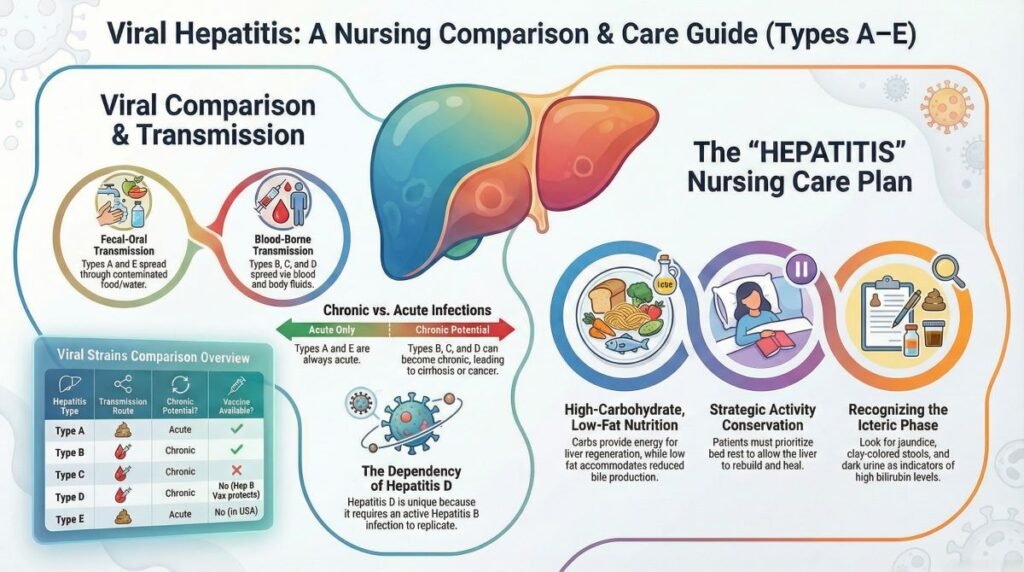
Hepatitis Symptoms: How to Recognize the Signs?
Many people with hepatitis, especially chronic forms, have no symptoms at all for years. When symptoms do appear, they may include:
- Fatigue and persistent tiredness
- Yellowing of the skin and eyes (jaundice)
- Dark urine (tea-coloured)
- Pale or clay-coloured stools
- Abdominal pain or discomfort, especially in the upper right side
- Nausea and vomiting
- Loss of appetite
- Fever (more common in acute hepatitis)
- Joint pain
- Itchy skin
Hepatitis symptoms in women may sometimes include irregular menstruation or hormonal disturbances, though these are less commonly discussed. Women are also more likely to develop autoimmune hepatitis than men.
Because symptoms can be mild or absent for long periods, regular testing is crucial if you are at risk.
Pathophysiology of Hepatitis: What Happens Inside the Liver
Understanding the pathophysiology of hepatitis helps explain why the disease is so serious. When the liver is infected or injured, the following process typically occurs:
- The hepatitis virus or harmful substance enters liver cells (hepatocytes) and begins replicating.
- The immune system detects the infected cells and sends inflammatory cells to attack them.
- This immune response causes liver cell death (necrosis) and inflammation.
- If inflammation is prolonged, it leads to fibrosis, where scar tissue replaces healthy liver cells.
- Extensive fibrosis leads to cirrhosis, which severely impairs liver function.
- In severe cases, cirrhosis can progress to liver failure or hepatocellular carcinoma (liver cancer).
This is why early diagnosis and treatment of hepatitis are so important.
Is Hepatitis Contagious? Who is at Risk?
Is hepatitis contagious? Yes, all viral forms of hepatitis are contagious to varying degrees. Here is a quick summary:
- Hepatitis A: Spreads through contaminated food and water (fecal-oral route). Highly contagious in environments with poor hygiene.
- Hepatitis B: Spreads through blood, sexual contact, and from mother to child. Is hepatitis B contagious through casual contact? No. You cannot get it from hugging, sharing food, or using the same toilet.
- Hepatitis C: Spreads mainly through blood. Less commonly through sex.
- Hepatitis D: Only spreads to those already infected with hepatitis B.
- Hepatitis E: Spreads through contaminated water. Not typically transmitted person to person.
How is Hepatitis Diagnosed?
How is hepatitis diagnosed? A doctor uses a combination of blood tests, imaging, and sometimes a liver biopsy.
Blood Tests
Blood tests are the foundation of hepatitis diagnosis. They include:
- Liver function tests (LFTs): Measure enzymes like ALT and AST that are elevated when the liver is inflamed.
- Hepatitis serology panels: Identify which virus is causing the infection, or whether you have immunity.
- Viral load tests (PCR): Measure the amount of virus in the blood, important for monitoring treatment.
- Hepatitis B antigen and antibody tests: Identify current infection (antigen) or immunity (antibody).
Imaging Tests
Ultrasound, CT scan, or MRI can assess the size and texture of the liver and detect complications such as cirrhosis or tumours.
FibroScan (Elastography)
This non-invasive test measures liver stiffness, which indicates the amount of fibrosis or scarring.
Liver Biopsy
In some cases, a small sample of liver tissue is taken for analysis under a microscope. This provides detailed information about the degree of inflammation and fibrosis.
Is Hepatitis Curable? What You Need to Know
Is hepatitis curable? The answer depends on the type:
- Hepatitis A: Fully curable. There is no specific treatment. The body clears the infection on its own, usually within a few weeks.
- Hepatitis B: Not always curable, but manageable. Antiviral medications can suppress the virus and prevent liver damage. A functional cure (clearing the surface antigen) is possible in a minority of patients.
- Hepatitis C: Highly curable. Modern direct-acting antiviral (DAA) medications cure over 95 percent of cases within 8 to 12 weeks.
- Hepatitis D: Difficult to cure. Emerging treatments like bulevirtide show promise.
- Hepatitis E: Curable. Most people recover without treatment in a few weeks.
Is hepatitis deadly? It can be, if left untreated. Chronic hepatitis B and C are among the leading causes of liver cancer worldwide. However, with early diagnosis and proper treatment, most people with hepatitis can live long, healthy lives.
Hepatitis Treatment: Medications and Options Available Today
Hepatitis treatment has advanced significantly in the last decade. Here is an overview of the most effective options:
Treatment for Hepatitis A and E
There is no specific antiviral treatment for hepatitis A or E. Management focuses on rest, adequate hydration, avoiding alcohol and drugs that strain the liver, and monitoring symptoms until the infection resolves.
Treatment for Hepatitis B
Antiviral drugs are used to reduce viral replication and prevent liver damage. Common medications include:
- Tenofovir (TDF or TAF)
- Entecavir
- Pegylated interferon alfa (for eligible patients)
These do not always clear the virus but they control it effectively. Xifaxan for liver (rifaximin) is also sometimes used in hepatitis B patients with complications like hepatic encephalopathy to reduce ammonia-producing bacteria in the gut.
Treatment for Hepatitis C: Harvoni, Epclusa, and Mavyret
Hepatitis C treatment has been revolutionised by direct-acting antivirals (DAAs). These are oral medications taken once daily for 8 to 12 weeks with a cure rate above 95 percent. The most well-known options include:
Harvoni (Ledipasvir/Sofosbuvir)
Harvoni is an oral tablet used to treat chronic hepatitis C genotype 1, which is the most common genotype in many countries. It is taken once a day and is generally well-tolerated. Harvoni cost can be significant without insurance, often ranging from tens of thousands of dollars for a full course in the United States. However, generic versions are widely available in many countries at a fraction of the Harvoni price. Patients should check their insurance coverage and explore patient assistance programs.
Epclusa (Sofosbuvir/Velpatasvir)
Epclusa is a pan-genotypic direct-acting antiviral, meaning it works across all hepatitis C genotypes (1 through 6). This makes it a very versatile treatment option. Epclusa is taken as one tablet once a day for 12 weeks. Epclusa cost in the United States can also be high without insurance, but generic versions are available in many parts of the world. Patients should ask their provider about financial assistance if Epclusa cost is a concern.
Mavyret (Glecaprevir/Pibrentasvir)
Mavyret is another pan-genotypic hepatitis C treatment. It is often prescribed for 8 weeks in patients without cirrhosis and has a very high cure rate. It is taken as three tablets once daily with food.
Treatment for Hepatitis D
Hepatitis D treatment remains challenging. Options currently in use or being studied include:
- Bulevirtide: A newer entry inhibitor approved in Europe. Bulevirtide works by blocking the virus from entering liver cells, and it has shown significant reductions in HDV viral load in clinical trials.
- Pegylated interferon alfa-2a: Used for 48 to 72 weeks, though it has significant side effects.
If you or someone you know has hepatitis D, it is important to work with a liver specialist familiar with the latest hepatitis D treatments and clinical trials.
Hepatitis and Liver Health: The Role of Xifaxan
Xifaxan (rifaximin) is an antibiotic sometimes prescribed for people with advanced liver disease. While it is not a direct antiviral for hepatitis, xifaxan for liver patients is used to manage hepatic encephalopathy, a brain condition caused by the liver’s inability to filter toxins like ammonia. It works by reducing ammonia-producing bacteria in the gut, helping to keep the mind clear in patients with cirrhosis.
Prevention of Hepatitis
Prevention is always better than cure, and many forms of hepatitis are entirely preventable:
Vaccination
- Hepatitis A vaccine: Two doses, provides long-term protection.
- Hepatitis B vaccine: Three doses, provides lifelong immunity for most people. Since hepatitis D can only infect those with hepatitis B, the hepatitis B vaccine also protects against hepatitis D.
Safe Practices
- Practice safe sex. Use condoms to reduce the risk of hepatitis B and C transmission.
- Never share needles, syringes, or drug-use equipment.
- Avoid sharing personal items like razors or toothbrushes.
- Ensure medical and dental equipment is properly sterilised.
- Drink clean, safe water to prevent hepatitis A and E.
- Wash hands thoroughly before eating and after using the toilet.
When Should You Get Tested for Hepatitis?
You should talk to your doctor about hepatitis testing if you:
- Were born between 1945 and 1965 (hepatitis C testing is recommended for this group)
- Have ever injected drugs, even once
- Have had unprotected sex with multiple partners
- Received a blood transfusion before 1992
- Are pregnant (hepatitis B screening is standard)
- Have elevated liver enzymes on a routine blood test
- Have a family member with hepatitis B or C
- Were born in a country where hepatitis B is common
Living with Hepatitis: Managing Your Health
A diagnosis of hepatitis does not have to be life-defining. With the right care, most people with hepatitis can live full, active lives. Here are some practical steps:
- Work closely with a hepatologist or gastroenterologist.
- Attend regular follow-up appointments and blood tests.
- Avoid alcohol entirely, as it worsens liver inflammation.
- Eat a balanced, liver-friendly diet low in saturated fats and processed foods.
- Maintain a healthy weight to avoid fatty liver complications.
- Avoid unnecessary medications and supplements that are processed by the liver.
- Stay up to date with hepatitis A and B vaccinations if you have hepatitis C.
- Do not donate blood, organs, or tissue.
- Inform sexual partners and healthcare providers of your diagnosis.
What is Hepatitis? Complete Reference Tables
These tables provide a quick, comprehensive reference to all types of hepatitis – covering viruses, real-life examples, symptoms, contagiousness, curability, and treatments. Use these alongside the full blog article for a complete picture.
Note: All examples are illustrative, representative of real-world scenarios. Consult a qualified healthcare professional for personal medical advice.
Table 1: Complete Comparison of All Hepatitis Types – Virus, Symptoms, Cure & Treatment
| Type | Virus | How It Spreads | Real-Life Example | Key Symptoms | Acute / Chronic | Contagious? | Curable? | Treatment / Medicines |
| Hepatitis A | HAV (Hepatitis A Virus) | Contaminated food or water (fecal-oral route) | A family in Delhi gets sick after eating at a street stall with poor sanitation. Three members develop jaundice within 4 weeks. | Jaundice, fever, nausea, fatigue, dark urine, loss of appetite, abdominal pain | Acute only (no chronic form) | Yes – highly contagious through food/water | Yes – fully self-curable. No antiviral needed. | Rest, fluids, avoid alcohol. Hepatitis A vaccine prevents infection. |
| Hepatitis B | HBV (Hepatitis B Virus) | Blood, sexual contact, mother to baby at birth, sharing needles/razors | A 32-year-old nurse accidentally gets a needlestick from an infected patient. Blood test shows HBsAg reactive. She begins antiviral therapy immediately. | Jaundice, fatigue, joint pain, dark urine, pale stools, nausea, abdominal pain. Many have NO symptoms for years. | Can be Acute or Chronic (chronic in ~5–10% of adults; ~90% of newborns) | Yes – spreads through blood and body fluids, NOT through casual contact | Not always fully cured, but highly manageable. Some achieve functional cure. | Tenofovir (TDF/TAF), Entecavir, Pegylated Interferon. Hepatitis B vaccine (3 doses) prevents infection. |
| Hepatitis C | HCV (Hepatitis C Virus) | Blood-to-blood contact – shared needles, unscreened blood transfusions, rarely sexual | A 45-year-old man in Mumbai donated blood and was told his HCV antibody test was positive. He had no symptoms. He was put on Epclusa for 12 weeks and achieved a cure (SVR12). | Often silent for years. When symptoms appear: fatigue, jaundice, dark urine, nausea, joint pain, brain fog (hepatic encephalopathy in advanced disease) | Usually becomes Chronic (~75–85% of cases) | Yes, but mainly through blood. Low risk through sex. | YES – >95% cure rate with Direct-Acting Antivirals (DAAs) | Epclusa (Sofosbuvir/Velpatasvir) – pan-genotypic, 12 weeks. Harvoni (Ledipasvir/Sofosbuvir) – for genotype 1, 12 weeks. Mavyret (Glecaprevir/Pibrentasvir) – pan-genotypic, 8–12 weeks. |
| Hepatitis D | HDV (Hepatitis D Virus / D virus / Delta virus) | Only infects those already infected with Hepatitis B. Spreads via blood and sexual contact. | A 38-year-old man with chronic hepatitis B develops a sudden severe worsening of liver function. Further testing reveals a hepatitis D superinfection. He is enrolled in a bulevirtide clinical trial. | Fatigue, jaundice, liver pain, rapid progression to cirrhosis. Often more severe than Hepatitis B alone. | Can be Acute (co-infection with HBV) or Chronic (superinfection in HBV carriers) | Yes – through blood and body fluids (only if patient already has HBV) | Difficult to cure. Newer treatments show significant promise. | Bulevirtide (entry inhibitor, approved in Europe) – blocks virus from entering liver cells. Pegylated Interferon Alfa-2a (48–72 weeks). Hepatitis B vaccine also prevents Hepatitis D. |
| Hepatitis E | HEV (Hepatitis E Virus) | Contaminated drinking water (fecal-oral route). Rare person-to-person spread. | During monsoon season in a rural area of Bihar, a local well becomes contaminated with sewage. 15 villagers develop jaundice within 3 weeks. A pregnant woman among them is hospitalised with acute liver failure. | Jaundice, fever, fatigue, nausea, vomiting, abdominal pain, dark urine. Extremely dangerous in pregnant women. | Usually Acute. Can become chronic in immunocompromised patients. | Yes – through contaminated water. Not typically person-to-person. | Yes – most people recover fully in 4–6 weeks without treatment. | Rest, hydration, avoid alcohol and hepatotoxic drugs. Ribavirin used in chronic cases or immunocompromised patients. Vaccine available in China (not widely approved elsewhere). |
| Alcoholic Hepatitis | NOT a virus – caused by heavy, long-term alcohol use | NOT contagious. Caused by excessive alcohol consumption damaging liver cells. | A 50-year-old man who drank a bottle of whisky daily for 20 years is admitted to hospital with jaundice, swollen abdomen, and confusion. Liver biopsy confirms alcoholic hepatitis with early cirrhosis. | Jaundice, abdominal swelling (ascites), fever, nausea, vomiting, confusion (hepatic encephalopathy), elevated liver enzymes | Both – Acute (sudden heavy drinking) or Chronic (years of heavy use) | NO – not contagious at all | Depends on severity. Mild cases can reverse with abstinence. Severe cases may require liver transplant. | Complete alcohol abstinence (most critical). Corticosteroids (Prednisolone) for severe cases. Nutritional support. Xifaxan for liver (Rifaximin) to manage hepatic encephalopathy. Liver transplant in end-stage disease. |
| Autoimmune Hepatitis | NOT a virus – the immune system attacks the liver’s own cells | NOT contagious. Linked to genetic factors and other autoimmune diseases. | A 28-year-old woman with lupus begins developing jaundice and fatigue. Blood tests show very high liver enzymes and positive ANA (antinuclear antibodies). Liver biopsy confirms autoimmune hepatitis. | Fatigue, jaundice, abdominal discomfort, joint pain, enlarged liver, skin rashes, amenorrhea (in women) | Usually Chronic, lifelong management required | NO – not contagious at all | Not curable but very manageable with lifelong treatment. Remission is possible. | Prednisone (corticosteroid) to suppress immune attack. Azathioprine (to reduce steroid dose long-term). Regular monitoring of liver enzymes. Liver transplant if liver fails. |
Table 2: Hepatitis Lab Test Results Explained – What Each Test Means with Real-Life Examples
Here we coverd in this table: hepatitis B surface antigen reactive, hepatitis B surface antibody positive, hepatitis B reactive, hepatitis B non-reactive, hepatitis B antigen
| Test Name | What It Detects | Positive / Reactive Means | Negative / Non-Reactive Means | Real-Life Example |
| HBsAg (Hepatitis B Surface Antigen) | The outer protein coat of the Hepatitis B virus | HBsAg reactive = Active HBV infection. Virus is present. Patient is infectious. | HBsAg non reactive = No current HBV infection detected. | Rahul, 34, has a routine blood test before surgery. His HBsAg comes back reactive. Doctor refers him to a hepatologist for further assessment and antiviral treatment. |
| Anti-HBs (Hepatitis B Surface Antibody) | Antibodies against the HBV surface antigen – indicates immunity | HBsAb reactive / positive = Immune to HBV. Either vaccinated or recovered from past infection. | No detectable immunity. May need vaccination. | Priya got her 3-dose hepatitis B vaccine. Her anti-HBs test shows hepatitis B surface antibody reactive – she is now fully protected. |
| HBeAg (Hepatitis B e-Antigen) | Active viral replication inside liver cells | High viral activity. Patient is highly infectious. | Viral replication may be low or in immune control phase. | A patient with chronic HBV has HBeAg positive – doctor knows the virus is actively multiplying and begins antiviral therapy. |
| Anti-HBe (Hepatitis B e-Antibody) | Immune response to HBeAg | Immune system is responding. May indicate reduced viral activity. | Early or active phase infection. | A patient transitions from HBeAg positive to anti-HBe positive – a sign of seroconversion, meaning treatment is working. |
| Anti-HBc (Hepatitis B Core Antibody) | Past or current HBV infection history | Previous or ongoing exposure to HBV. Does not indicate immunity alone. | No prior exposure to HBV. | A blood donor tests anti-HBc positive but HBsAg negative – this suggests a past resolved infection. |
| HCV Antibody (Anti-HCV) | Antibodies to Hepatitis C virus | Past or current HCV infection. Needs confirmatory HCV RNA test. | No HCV exposure. | A 48-year-old gets tested during a health camp. Anti-HCV comes back positive. HCV RNA test confirms active infection – she is started on Epclusa. |
| HCV RNA (Viral Load) | Amount of Hepatitis C virus in blood | Active HCV infection. Quantifies how much virus is present. | No detectable virus. May indicate cure or resolved infection. | After 12 weeks of Mavyret treatment, patient’s HCV RNA is undetectable – this confirms a Sustained Virologic Response (SVR) – a cure. |
| ALT / AST (Liver Enzymes) | Liver cell damage and inflammation | Elevated levels = liver is inflamed or damaged | Normal = liver cells are intact | A patient with alcoholic hepatitis has ALT 10x above normal. Doctor knows liver damage is significant and advises immediate alcohol cessation. |
| Bilirubin | Breakdown product of red blood cells – filtered by liver | High bilirubin = liver cannot process waste properly, causing jaundice | Normal bilirubin = liver clearing waste efficiently | A patient with hepatitis A has bilirubin of 8 mg/dL (normal is under 1.2). Skin and eyes appear yellow – jaundice. |
Table 3: Hepatitis Medicines & Treatments – How They Work, Duration, Cure Rates & Cost
Here we Covers: Epclusa, Harvoni, Mavyret, Bulevirtide, Tenofovir, Entecavir, Pegylated Interferon, Ribavirin, Prednisolone, Xifaxan for liver
| Medicine | Hepatitis Type | How It Works | Duration | Cure Rate | Notes / Cost |
| Epclusa (Sofosbuvir + Velpatasvir) | Hepatitis C (all genotypes 1–6) | Blocks HCV RNA polymerase and NS5A protein – stops the virus from replicating | 12 weeks (1 tablet daily) | >95% cure (SVR12) | Pan-genotypic – works for all HCV genotypes. Epclusa cost in USA: ~$74,000 without insurance. Generic versions widely available in India and other countries at significantly lower Epclusa price. |
| Harvoni (Ledipasvir + Sofosbuvir) | Hepatitis C Genotype 1 | Dual action – blocks NS5A protein and NS5B polymerase of HCV | 12 weeks (1 tablet daily) | >94% cure rate | Harvoni is one of the most prescribed HCV treatments globally. Harvoni cost in USA can exceed $90,000 without coverage. Patients should check insurance and assistance programs. Generic Harvoni price is far lower in India. |
| Mavyret (Glecaprevir + Pibrentasvir) | Hepatitis C (all genotypes 1–6) | Inhibits two different HCV proteins (NS3/4A protease and NS5A) simultaneously | 8 weeks for non-cirrhotic patients; 12–16 weeks for cirrhotic | >97% in most genotypes | Shortest treatment course available for most patients. Taken as 3 tablets once daily with food. |
| Tenofovir (TDF / TAF) | Hepatitis B (chronic) | Nucleotide analogue – mimics DNA building blocks to stop HBV from replicating | Lifelong or long-term (years) | Suppresses virus, rarely clears it completely | First-line treatment for chronic HBV. TAF (Tenofovir Alafenamide) has fewer kidney and bone side effects than TDF. |
| Entecavir | Hepatitis B (chronic) | Guanosine analogue – blocks HBV DNA polymerase, preventing viral replication | Lifelong or long-term | Excellent viral suppression. HBsAg clearance rare. | Highly effective with low resistance rates. Preferred for HBV patients with no prior antiviral treatment. |
| Bulevirtide | Hepatitis D (HDV) | Entry inhibitor – blocks the NTCP receptor on liver cells that HDV uses to enter | 48 weeks+ (ongoing trials) | Significant reduction in HDV RNA in clinical trials. Full cure rates still being studied. | Approved in Europe (2020). First-ever specific treatment for HDV. Bulevirtide is a major breakthrough for hepatitis D treatments. Not yet FDA approved in USA. |
| Pegylated Interferon Alfa-2a | Hepatitis B, C, D | Boosts the immune system’s antiviral response and has direct antiviral effects | 24–72 weeks depending on type and response | HBV: ~30% sustained response. HDV: ~25–30% SVR. | Injected weekly. Significant side effects: flu-like symptoms, depression, fatigue. Less commonly used for HCV now due to superior DAA options. |
| Ribavirin | Hepatitis C (with interferon, older regimen) / Hepatitis E (chronic in immunocompromised) | Broad-spectrum antiviral – disrupts viral RNA synthesis | 24–48 weeks (HCV). 3–6 months (HEV). | Moderate – rarely used alone for HCV today | Largely replaced by DAAs for HCV. Still used for severe/chronic HEV in immunocompromised patients (e.g., organ transplant recipients). |
| Prednisolone (Corticosteroid) | Autoimmune Hepatitis | Suppresses the abnormal immune attack on liver cells | Long-term / lifelong | Achieves remission in ~80% of patients | Usually combined with Azathioprine to allow lower steroid dose. Regular monitoring for side effects including bone density, blood sugar. |
| Xifaxan (Rifaximin) | Hepatitis B/C/Alcoholic – advanced liver disease with hepatic encephalopathy | Antibiotic that reduces ammonia-producing gut bacteria, preventing brain toxicity | Ongoing – as long as risk persists | Not a cure for hepatitis – manages complications | Xifaxan for liver disease (particularly cirrhosis) reduces recurrence of hepatic encephalopathy by ~50%. It is an adjunct therapy, not a direct antiviral. |
Disclaimer: This document is for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your doctor or a qualified hepatologist before starting or changing any treatment.
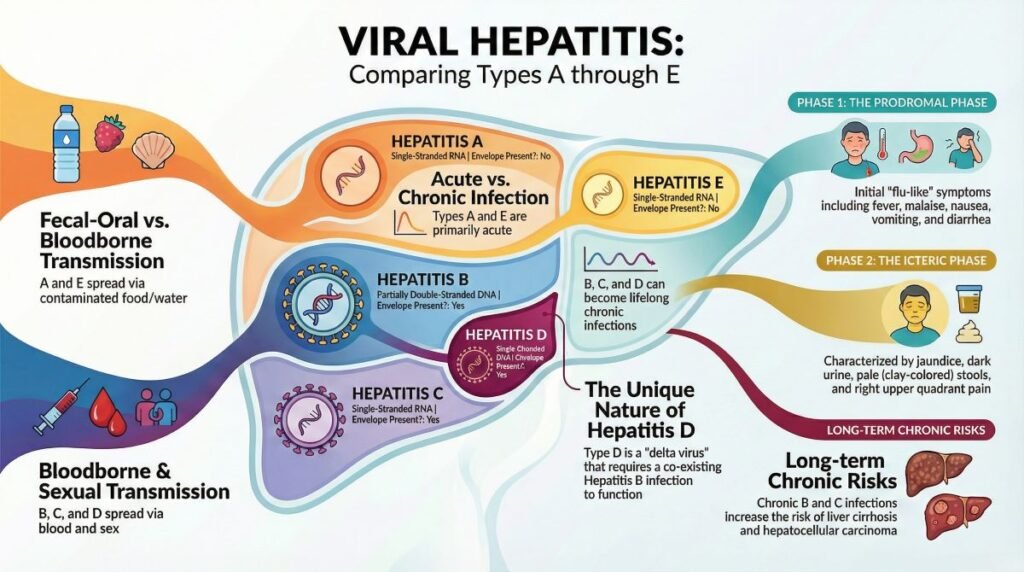
Table of Hepatitis
This table covers almost all Hepatitis related issues:
| # | Keyword | Category | Search Intent | What It Means / Brief Answer | How to Use in Article |
| ◆ MEDICINE / DRUG | |||||
| 1 | Harvoni cost | Medicine / Drug | Users researching the price of Harvoni (Ledipasvir/Sofosbuvir) for Hepatitis C treatment | Harvoni is a once-daily tablet for HCV genotype 1. In the USA, the list price can exceed $90,000 for a 12-week course without insurance. Generic versions are available in India and other countries at a fraction of the cost. Patients should check insurance and manufacturer assistance programs. | Include in Treatment section under Hepatitis C medicines. Compare branded vs generic pricing. |
| 2 | Harvoni price | Medicine / Drug | Same as above — users want to know the Harvoni price before purchasing or asking their doctor | Same as Harvoni cost. Harvoni price varies significantly by country. In India, generic ledipasvir/sofosbuvir is available for a few thousand rupees for a full course. | Use alongside ‘Harvoni cost’ — they are the same query with different phrasing. Mention both in article. |
| 3 | Epclusa cost | Medicine / Drug | Users want to know how much Epclusa (Sofosbuvir/Velpatasvir) costs before starting treatment | Epclusa is a pan-genotypic HCV treatment — works for genotypes 1–6. US list price is ~$74,000 for 12 weeks without coverage. Generic versions available widely in developing countries. | Mention Epclusa cost in HCV Treatment section. Pair with ‘Is Hepatitis C curable?’ content. |
| 4 | Epclusa | Medicine / Drug | Users want general information about what Epclusa is and what it treats | Epclusa (Sofosbuvir + Velpatasvir) is a direct-acting antiviral (DAA) for all HCV genotypes. Taken as one tablet daily for 12 weeks. Cure rate >95%. | Dedicate a subheading to Epclusa in the Treatment section. Explain pan-genotypic action. |
| 5 | Mavyret | Medicine / Drug | Users want to know what Mavyret is and whether it cures Hepatitis C | Mavyret (Glecaprevir + Pibrentasvir) is a pan-genotypic HCV treatment. Taken as 3 tablets once daily with food. 8-week course for non-cirrhotic patients. Cure rate >97%. | Add to HCV treatment section with comparison vs Epclusa and Harvoni. |
| 6 | Mavyret cost | Medicine / Drug | Users want to know Mavyret’s price before treatment decision | Mavyret US list price is approximately $26,000 for an 8-week course. Manufacturer AbbVie has patient assistance programs. Generic versions available in some countries. | Use in Treatment section. Compare cost-effectiveness with Epclusa and Harvoni. |
| 7 | Mavyret price | Medicine / Drug | Same intent as Mavyret cost — different phrasing | Same as Mavyret cost. Mention both keyword variants in article body or FAQ. | Pair with Mavyret cost paragraph — use both terms naturally. |
| 8 | Glecaprevir | Medicine / Drug | Users searching for the active ingredient in Mavyret (HCV treatment) | Glecaprevir is an NS3/4A protease inhibitor combined with Pibrentasvir (NS5A inhibitor) to form Mavyret. It blocks a key enzyme the Hepatitis C virus needs to replicate. | Mention in the Mavyret explanation. Helps SEO for users searching by active ingredient. |
| 9 | Bulevirtide | Medicine / Drug | Users want to know about the new Hepatitis D treatment Bulevirtide | Bulevirtide is the first-ever specifically approved treatment for chronic Hepatitis D (HDV). It is an entry inhibitor that blocks NTCP receptors, preventing HDV from entering liver cells. Approved in Europe in 2020. Not yet FDA-approved in the USA. | Dedicate a subheading in Hepatitis D Treatment section. Highlight as breakthrough drug. |
| 10 | Direct acting antivirals | Medicine / Drug | Users want to understand what DAAs are and how they work for Hepatitis C | Direct-acting antivirals (DAAs) are a class of medications that directly target proteins of the Hepatitis C virus (HCV). They include drugs like Epclusa, Harvoni, and Mavyret. They achieve >95% cure rate in 8–12 weeks. | Use in the HCV treatment intro. Define DAAs before listing individual drugs. |
| 11 | DAA HCV | Medicine / Drug | Short search for Direct-Acting Antivirals for Hepatitis C | DAA = Direct-Acting Antiviral. DAA HCV treatment has revolutionised Hepatitis C therapy with cure rates above 95% and minimal side effects compared to older interferon-based regimens. | Use as internal link anchor. Great for FAQ: ‘What are DAA HCV treatments?’ |
| 12 | DAA Hepatitis C | Medicine / Drug | Same as DAA HCV — longer phrasing | Same intent as DAA HCV. Include both natural variations in the HCV treatment section. | Use naturally in HCV treatment paragraphs alongside ‘direct acting antivirals’. |
| 13 | Xifaxan for liver | Medicine / Drug | Users want to know how Rifaximin (Xifaxan) is used in liver disease management | Xifaxan (Rifaximin) is an antibiotic used to manage hepatic encephalopathy in patients with advanced liver disease or cirrhosis. It reduces ammonia-producing gut bacteria, preventing brain toxicity. Not a cure for hepatitis but manages complications. | Add to Advanced Liver Disease / Complications section after covering core treatments. |
| 14 | Thervacb | Medicine / Drug | Users searching for Thervacb — an investigational therapeutic vaccine for Hepatitis B | Thervacb (also written TherVacB) is an experimental therapeutic vaccine being developed to cure chronic Hepatitis B. It is in clinical trials and aims to trigger an immune response to clear HBV. Not yet commercially available. | Mention in ‘Future of Hepatitis B Treatment’ or Emerging Therapies section. |
| ◆ LAB TEST / RESULT | |||||
| 15 | Hepatitis B surface antigen reactive | Lab Test / Result | Patients who received a lab result and want to know what it means | HBsAg reactive means the Hepatitis B surface antigen is detected in the blood. This indicates an active, current Hepatitis B infection. The patient can transmit the virus to others. Immediate medical consultation is needed. | Create a dedicated ‘Understanding Your Hepatitis B Lab Results’ section. This is a high-value query. |
| 16 | Hepatitis B surface antigen positive | Lab Test / Result | Same as reactive — users use ‘positive’ and ‘reactive’ interchangeably | Same meaning as HBsAg reactive. The virus is present in the blood. Patient has Hepatitis B. Both ‘positive’ and ‘reactive’ are used in different lab reports globally. | Use both terms (reactive/positive) together in the article to capture both keyword variants. |
| 17 | Hepatitis B surface antigen non reactive | Lab Test / Result | Patients who got a non-reactive result and want to understand it | HBsAg non reactive means the Hepatitis B surface antigen was NOT detected. No active Hepatitis B infection at the time of testing. This is the desired/normal result. | Address in the lab results section. Reassure readers what non-reactive means. |
| 18 | Hepatitis B surface antigen negative | Lab Test / Result | Same as non-reactive — patients want to confirm negative = good | HBsAg negative = same as non-reactive. No virus detected. However, further tests (anti-HBc, anti-HBs) may still be needed to establish immunity status. | Use alongside ‘non reactive’ in the same paragraph for full keyword coverage. |
| 19 | Hepatitis B surface antibody reactive | Lab Test / Result | Patients who tested positive for surface antibody and want to understand the result | Anti-HBs reactive (surface antibody reactive) means the immune system has produced protective antibodies. This is a GOOD result — it indicates immunity against HBV, from either vaccination or recovery from past infection. | Include in lab results section. Clarify difference between surface antigen (infection) vs surface antibody (immunity). |
| 20 | Hepatitis B surface antibody positive | Lab Test / Result | Same intent — different lab report terminology | Same as surface antibody reactive. Patient is immune to Hepatitis B. Cannot be reinfected (in most cases). No treatment required for HBV. | Use both ‘reactive’ and ‘positive’ in same paragraph. These are interchangeable search terms. |
| 21 | Hepatitis B surface antibody | Lab Test / Result | Broad search — users want to understand what the surface antibody test is | The Hepatitis B surface antibody (anti-HBs or HBsAb) is a blood test marker that indicates immune response to HBV. It is measured after vaccination or during recovery. A level >10 mIU/mL is considered protective. | Define clearly in lab test section. Link to FAQ: ‘What does HBsAb mean?’ |
| 22 | Hepatitis B surface ab reactive | Lab Test / Result | Variant phrasing of surface antibody reactive | Hep B surface Ab (antibody) reactive = immune to Hepatitis B. ‘Ab’ is medical shorthand for antibody. Same meaning as anti-HBs positive or HBsAb reactive. | Use this exact phrase naturally in the article. Common on Indian lab reports. |
| 23 | Hepatitis B surface ab | Lab Test / Result | Short form search for Hepatitis B surface antibody | Hep B surface Ab = Hepatitis B surface antibody. A key marker in the Hepatitis B panel. Tests for immunity, not active infection. | Use as variation in same paragraph as ‘hepatitis b surface antibody’. |
| 24 | Hep bs ab | Lab Test / Result | Abbreviated search often used after reading a lab report | Hep Bs Ab = Hepatitis B surface antibody. The ‘s’ refers to ‘surface’. This test checks for antibodies (immunity) against the surface protein of HBV. | Include this exact abbreviation in article — many Indian lab reports use this format. |
| 25 | Hepatitis B antibody reactive | Lab Test / Result | Patients who got ‘hepatitis B antibody reactive’ on their lab report | Hepatitis B antibody reactive generally refers to the surface antibody (anti-HBs) being detected. Indicates immunity. However, context matters — it could also refer to core antibody (anti-HBc). Always clarify which antibody with your doctor. | Clarify the ambiguity in the article. Explain that ‘hepatitis B antibody’ can mean different things. |
| 26 | Hepatitis B antibody positive | Lab Test / Result | Same as antibody reactive — positive and reactive mean the same thing | Anti-HBs positive = immune to Hepatitis B. Good news for the patient. May not need vaccination or treatment. | Cover in the same paragraph as ‘antibody reactive’. These are synonym searches. |
| 27 | Hepatitis B antibody | Lab Test / Result | Broad search — users want to understand all HBV antibody tests | Hepatitis B antibodies include: anti-HBs (surface antibody = immunity), anti-HBc (core antibody = past exposure), and anti-HBe (e-antibody = reduced viral activity). Each tells a different story about the patient’s HBV status. | Create a mini table or list within the article explaining all three types of HBV antibodies. |
| 28 | Hepatitis B reactive | Lab Test / Result | Broad term — patients got a ‘reactive’ result on ANY hepatitis B marker | Hepatitis B reactive can mean any of the Hepatitis B markers came back positive. It needs context — which marker is reactive? HBsAg reactive means active infection. Anti-HBs reactive means immune. Doctor must interpret the full Hepatitis B panel. | Add to FAQ: ‘What does Hepatitis B reactive mean?’ — explain it depends on which test. |
| 29 | Hepatitis B non reactive | Lab Test / Result | Patients who got a non-reactive result and want reassurance | Hepatitis B non reactive means no active marker was detected for the specific test. For HBsAg non reactive = no infection. For Anti-HBs non reactive = no immunity detected (may need vaccine). Must consider full panel. | Address in lab section — pair with ‘reactive’ explanation. Very commonly searched. |
| 30 | Hepatitis B surface | Lab Test / Result | Broad search — users want info about HBV surface antigen/antibody | The Hepatitis B surface refers to the outer protein coat (envelope) of the HBV virus. Two key tests: (1) HBsAg = surface antigen (detects virus), (2) Anti-HBs = surface antibody (detects immunity). | Use as a bridge paragraph before explaining HBsAg and anti-HBs separately. |
| 31 | Hepatitis B antigen | Lab Test / Result | Users want to understand what a Hepatitis B antigen is | A hepatitis B antigen is a protein from the HBV virus that triggers an immune response. The main antigens are: HBsAg (surface antigen), HBeAg (e-antigen indicating replication), and HBcAg (core antigen). | Create a clear definitions box in the article. Very educational for readers. |
| 32 | Hepatitis B core antibody positive | Lab Test / Result | Patients who received a positive core antibody result | Anti-HBc positive (core antibody positive) means the person has been exposed to Hepatitis B at some point — past or present. It does NOT mean immunity (that’s anti-HBs). Positive core antibody in a blood donor can lead to deferral. | Add to lab results section. Distinguish clearly from surface antibody. |
| 33 | Hepatitis B core ab total | Lab Test / Result | Specific search for the ‘total’ core antibody test (includes IgM and IgG) | Hepatitis B core ab total (anti-HBc total) detects both IgM (acute infection) and IgG (past exposure) core antibodies. A positive total anti-HBc with negative HBsAg and positive anti-HBs = past resolved infection. A positive total anti-HBc with positive HBsAg = chronic infection. | Include in lab results table. Explain IgM vs IgG differentiation for acute vs chronic. |
| 34 | Hepatitis B core antigen | Lab Test / Result | Users want to know what the core antigen is and how it differs from surface antigen | The Hepatitis B core antigen (HBcAg) is found inside infected liver cells — it is NOT detectable in the blood directly. It triggers the production of anti-HBc antibodies. It is different from HBsAg (surface antigen), which IS detectable in blood. | Clarify in article: HBcAg is NOT a standard blood test result — anti-HBc (antibody to it) is what gets tested. |
| 35 | Hepatitis B core antibody | Lab Test / Result | Same as core antibody positive — users want to understand this test | Anti-HBc is the antibody the body produces against the Hepatitis B core antigen. Presence indicates past or current HBV exposure. Needs to be interpreted alongside other HBV markers. | Use consistently with ‘hepatitis B core ab’ — they mean the same thing. |
| 36 | Hepatitis B core ab | Lab Test / Result | Abbreviated version of core antibody — common lab report notation | Hep B core Ab = anti-HBc = Hepatitis B core antibody. Indicates past or current exposure to HBV. Must be interpreted with full panel. | Use this abbreviation naturally in the article to match common Indian lab report language. |
| 37 | Hepatitis be antibody | Lab Test / Result | Users want to understand the ‘e antibody’ (anti-HBe) in HBV panel | Anti-HBe (Hepatitis Be antibody or e-antibody) appears when HBeAg clears from the blood. This ‘seroconversion’ (HBeAg → anti-HBe) often indicates reduced viral replication and lower infectivity. A positive anti-HBe is generally a good sign in chronic HBV. | Explain HBeAg to anti-HBe seroconversion in the HBV section. Marks treatment response. |
| 38 | Hepatitis be antigen | Lab Test / Result | Users want to know about HBeAg and what it means for infection activity | HBeAg (Hepatitis B e-antigen) is a protein produced during active HBV replication. HBeAg positive = high viral replication = very infectious. Its presence drives decisions about starting antiviral treatment. | Mention alongside HBsAg in lab results section. Explain it as a marker of disease activity. |
| 39 | Hepatitis bs ab | Lab Test / Result | Abbreviated search for Hepatitis B surface antibody | Hep Bs Ab = Hepatitis B surface antibody (anti-HBs). The ‘s’ = surface, ‘ab’ = antibody. Reactive/positive = immune to HBV. | Common abbreviation on Indian lab reports. Include in article to target this exact search. |
| 40 | Hepatitis B virus surface ab | Lab Test / Result | Full phrasing for the surface antibody test | Hepatitis B virus surface Ab = anti-HBs = surface antibody. Positive indicates immunity. Key marker to confirm successful vaccination. | Use this full phrase once in article to capture long-tail search traffic. |
| 41 | Hepatitis B panel | Lab Test / Result | Users want to know what tests are included in a hepatitis B panel | A standard Hepatitis B panel includes: HBsAg (surface antigen), anti-HBs (surface antibody), and anti-HBc (core antibody). Extended panels may include HBeAg, anti-HBe, and HBV DNA/viral load. Ordered together to assess infection status, immunity, and exposure history. | Create a ‘What is a Hepatitis B Panel?’ section or table. High informational value. |
| 42 | Hepatitis panel quest | Lab Test / Result | Users looking for Hepatitis B panel on Quest Diagnostics (major US lab) | Quest Diagnostics offers several hepatitis panels. The Hepatitis B Panel (#7902) includes HBsAg, anti-HBs, and anti-HBc. Always consult your doctor on which panel is right for your situation. | Useful for US audience. Mention Quest as a well-known lab in a parenthetical note. |
| 43 | HAV test | Lab Test / Result | Users want to know how Hepatitis A is tested | HAV test detects Hepatitis A antibodies in the blood. HAV IgM positive = current or recent HAV infection. HAV IgG positive = past infection or successful vaccination (immunity). | Include in Hepatitis A section. Brief explanation of what the HAV test tells you. |
| 44 | Hepatitis C antibody non reactive | Lab Test / Result | Patients who got a non-reactive HCV antibody result | HCV antibody non reactive = no detectable antibodies to Hepatitis C. This is the desired/normal result. However, if infection was very recent (within 8–11 weeks), antibodies may not yet be detectable — repeat testing may be needed. | Mention in Hepatitis C testing section. Note the ‘window period’ for antibody detection. |
| 45 | Hepatitis C antibody reactive | Lab Test / Result | Patients who got a reactive HCV antibody result and want to understand it | HCV antibody reactive means the body has been exposed to Hepatitis C virus at some point. It does NOT confirm active infection. A confirmatory HCV RNA (PCR) test is needed to determine if the virus is still present. | Critical distinction — explain the two-step HCV testing process clearly in article. |
| 46 | Hepatitis C antibody positive | Lab Test / Result | Same as reactive — patients use both terms for the same result | Same as HCV antibody reactive. Indicates past or present HCV exposure. Requires HCV RNA test to confirm active infection. A positive antibody with negative RNA may mean the person cleared the infection naturally. | Use both ‘reactive’ and ‘positive’ in same paragraph for comprehensive keyword coverage. |
| 47 | Hepatitis C ab | Lab Test / Result | Abbreviated search for Hepatitis C antibody test | HCV Ab = Hepatitis C antibody. Standard initial screening test for HCV. Reactive/positive result requires follow-up RNA testing. | Use this abbreviation in the lab testing section. Common medical shorthand. |
| 48 | Hepatitis B viral load | Lab Test / Result | Patients want to understand their HBV viral load test result | Hepatitis B viral load (HBV DNA test) measures the amount of Hepatitis B virus in the blood. High viral load = active replication, higher liver damage risk, and often an indication to start antiviral treatment. Monitored regularly during treatment. | Include in Hepatitis B monitoring section. Explain how viral load guides treatment decisions. |
| 49 | Hepatitis C viral load | Lab Test / Result | Patients want to understand their HCV viral load result | Hepatitis C viral load (HCV RNA quantitative test) measures how much HCV is in the blood. It is used to confirm active infection, guide treatment, and assess cure. An undetectable viral load 12 weeks after treatment = SVR12 = cure. | Include in Hepatitis C section. Explain SVR12 as the definition of a hepatitis C cure. |
| ◆ HEPATITIS B | |||||
| 50 | Acute hepatitis B | Hepatitis B | Users want to understand acute (short-term) Hepatitis B infection | Acute Hepatitis B is a short-term infection lasting less than 6 months. Most adults (>90%) naturally clear the virus and develop immunity. Symptoms include jaundice, fatigue, and nausea. It becomes chronic if the virus persists beyond 6 months. | Add to the Hepatitis B section. Contrast acute vs chronic to help readers understand their diagnosis. |
| 51 | Chronic hepatitis B | Hepatitis B | Users want to understand long-term Hepatitis B and its consequences | Chronic Hepatitis B persists beyond 6 months. It occurs in ~5–10% of adults infected, and ~90% of infants infected at birth. Without treatment, it can lead to cirrhosis, liver failure, or liver cancer over decades. Long-term antiviral therapy is the standard of care. | Make chronic hepatitis B a key focus. Many readers with chronic HBV will search this. |
| 52 | Stages of hepatitis B | Hepatitis B | Users want to know how chronic Hepatitis B progresses over time | Chronic HBV has 4 phases: (1) Immune Tolerant — high viral load, normal liver enzymes, (2) Immune Active — high viral load, elevated enzymes, liver inflammation, (3) Inactive Carrier — low viral load, normal enzymes, (4) HBeAg-negative Hepatitis — reactivation phase. Treatment decisions depend on the phase. | Add a ‘Stages of Hepatitis B’ section or table. Very high informational value for diagnosed readers. |
| 53 | Hepatitis B is caused by | Hepatitis B | Basic educational search — readers want to know the root cause of HBV | Hepatitis B is caused by the Hepatitis B virus (HBV), a double-stranded DNA virus of the Hepadnaviridae family. It is transmitted through blood, sexual contact, and from mother to child at birth. | Address in introduction or early in Hepatitis B section. Fundamental SEO keyword. |
| 54 | Hepatitis B is transmitted by | Hepatitis B | Readers want to know exactly how Hepatitis B spreads | Hepatitis B is transmitted by: (1) blood-to-blood contact, (2) unprotected sex with an infected person, (3) mother to baby during birth, (4) sharing needles or sharp instruments, (5) needlestick injuries. NOT transmitted by casual contact, sharing food, hugging, or coughing. | Answer clearly with a bulleted list. Address common misconceptions about casual contact. |
| 55 | Hepatitis B in pregnancy | Hepatitis B | Pregnant women or partners concerned about HBV risk during pregnancy | Hepatitis B in pregnancy poses a high risk of mother-to-child transmission (vertical transmission) — up to 90% if mother is HBeAg positive. All pregnant women should be screened. Babies born to HBsAg-positive mothers should receive HBIG and first HBV vaccine within 12 hours of birth. | Add a ‘Hepatitis B and Pregnancy’ section. Very important for audience in India where HBV is endemic. |
| 56 | Hepatitis B carrier | Hepatitis B | Users want to know what it means to be a Hepatitis B carrier | A Hepatitis B carrier is someone who has been HBsAg positive for more than 6 months (chronic infection) but may have minimal liver inflammation (inactive carrier state). Carriers can still transmit HBV to others. Regular monitoring is essential. | Define ‘carrier’ clearly in article. Reassure readers while explaining monitoring needs. |
| 57 | Hepatitis B precautions | Hepatitis B | Readers who have HBV or live with someone who has HBV want to know safety steps | Hepatitis B precautions include: (1) vaccination of all household and sexual contacts, (2) using condoms, (3) not sharing razors, toothbrushes, or needles, (4) covering open wounds, (5) informing healthcare providers. The virus is NOT spread through casual contact. | Add a ‘Living with Hepatitis B: Precautions’ section. Practical value for caregivers. |
| 58 | My husband has hepatitis B can I get it | Hepatitis B | Partners of HBV patients worried about their own risk of infection | Yes, Hepatitis B can be transmitted sexually. If your husband has HBV, you should: (1) get tested for Hepatitis B immediately, (2) get vaccinated if not already immune, (3) use condoms until you have confirmed immunity. HBV is NOT spread through hugging, kissing on cheek, or sharing meals. | Write a specific FAQ addressing this concern. Highly empathetic entry point for readers. |
| 59 | Hepatitis B sexually transmitted | Hepatitis B | Users want to know if Hepatitis B is an STI/STD | Yes, Hepatitis B is considered a sexually transmitted infection (STI). It can be spread through unprotected vaginal, anal, or oral sex. It is actually much more infectious than HIV through sexual contact. Vaccination and condom use are key preventive measures. | Include in Transmission section. Many readers may not know HBV is sexually transmitted. |
| 60 | Hepatitis B saliva | Hepatitis B | Users want to know if HBV can spread through saliva — e.g., kissing, sharing food | Hepatitis B virus has been found in saliva, but casual contact (kissing, sharing cutlery or cups) is NOT considered a significant route of transmission. The virus must enter the bloodstream or mucous membranes in significant quantity. Deep kissing with open sores may carry a small risk. | Add to Transmission FAQ. Many people worry about sharing food — address this directly. |
| 61 | Hepatitis B surface | Hepatitis B | Users searching broadly for information about the HBV surface | (Duplicate — covered under Lab Test/Result section.) Refers to the surface proteins of HBV including HBsAg and anti-HBs. Core concept for understanding HBV serology. | Already covered — ensure content is internally cross-linked within the article. |
| 62 | Hepatitis spread | Hepatitis B | General search about how hepatitis spreads | Hepatitis spread depends on the type: Hep A & E spread through contaminated food/water. Hep B, C, D spread through blood, sexual contact, or shared needles. Hep B also spreads from mother to baby. None spread through casual everyday contact. | Cover in a universal ‘How Does Hepatitis Spread?’ section near the top of the article. |
| ◆ HEPATITIS C | |||||
| 63 | Hepatitis C genotype | Hepatitis C | HCV patients want to understand genotypes and how they affect treatment | Hepatitis C has 6 major genotypes (1–6) and multiple subtypes. Genotype 1 is most common globally. Genotype 3 is most prevalent in South Asia. Genotype affects which medications are used (though pan-genotypic drugs like Epclusa and Mavyret work for all). Genotype testing is done via a blood test. | Add ‘Hepatitis C Genotypes’ subsection in HCV chapter. Crucial for treatment planning explanation. |
| 64 | HCV infection | Hepatitis C | Users searching for general information about Hepatitis C infection | HCV (Hepatitis C Virus) infection is a blood-borne viral infection. Most people develop chronic HCV if untreated. About 58 million people globally have chronic HCV. It is now highly curable with DAA medications. | Use ‘HCV infection’ naturally in the Hepatitis C overview section. |
| 65 | Hepatitis C precautions | Hepatitis C | People with HCV or their contacts want to know how to prevent spreading it | Hepatitis C precautions: (1) never share needles or syringes, (2) avoid sharing personal care items (razors, nail clippers), (3) cover cuts and sores, (4) healthcare workers should follow standard precautions. There is no vaccine for HCV, making personal precautions critical. | Add ‘Hepatitis C Precautions’ to living-with-hepatitis section or prevention section. |
| 66 | Hepatitis C treatment cost | Hepatitis C | Patients worried about being able to afford HCV treatment | HCV treatment cost varies widely. In the USA, branded DAAs (Epclusa, Harvoni, Mavyret) can cost $26,000–$90,000+ without insurance. In India and other countries, high-quality generics are available for as low as a few thousand rupees. Government programs, Medicaid, and manufacturer assistance programs can help. | Address cost concern directly in treatment section. Include both US pricing and generic alternatives. |
| 67 | Hepatitis C cure | Hepatitis C | Patients want to confirm HCV is actually curable | Yes, Hepatitis C is curable. Modern Direct-Acting Antivirals (DAAs) cure over 95% of HCV patients in 8–12 weeks. SVR12 (undetectable viral load 12 weeks post-treatment) is defined as a cure. This is one of the most significant medical achievements of the 21st century. | Highlight in HCV section with confidence. Many readers are anxious — reassure them clearly. |
| 68 | Hepatitis C rash | Hepatitis C | HCV patients experiencing skin symptoms want to know if rash is related | Hepatitis C can cause skin manifestations including: (1) lichen planus (itchy, flat-topped lesions), (2) porphyria cutanea tarda (blistering rash on sun-exposed skin), (3) cryoglobulinemia-related purpura (purple skin spots). These are extra-hepatic (outside the liver) manifestations of HCV. | Add ‘Hepatitis C and Skin Symptoms’ to the symptoms section. Many readers notice rash before liver symptoms. |
| 69 | CDC hepatitis C | Hepatitis C | Users looking for CDC guidelines or statistics on Hepatitis C | The US Centers for Disease Control and Prevention (CDC) recommends universal HCV screening for all adults aged 18 and older at least once, and for all pregnant women during every pregnancy. The CDC estimates 2.4 million people in the US live with Hepatitis C. | Reference CDC as an authoritative source. Add to Prevention/Screening section for credibility. |
| 70 | HIV and hepatitis | Hepatitis C | Users want to know about the relationship between HIV and viral hepatitis | HIV and Hepatitis C (HCV) coinfection is common because they share transmission routes (blood, sexual contact). People living with HIV are at higher risk of rapid liver disease progression if coinfected with HBV or HCV. DAA treatment is safe and effective in HIV-HCV coinfected patients. Antiretroviral therapy (ART) for HIV can also help control Hepatitis B. | Add an ‘HIV and Hepatitis’ section or FAQ. Important for risk populations. |
| 71 | Serum hepatitis | Hepatitis C | Users may have encountered this older medical term | Serum hepatitis is an outdated term historically used for Hepatitis B (transmitted through blood/serum). The term was used before the virus was identified. Modern terminology uses ‘Hepatitis B’ instead. | Mention briefly in the Hepatitis B history paragraph or a footnote. |
| ◆ HEPATITIS D | |||||
| 72 | Hepatitis D treatment | Hepatitis D | HDV patients or doctors searching for treatment options | Hepatitis D treatment options include: (1) Bulevirtide — first approved HDV-specific drug (Europe, 2020), (2) Pegylated Interferon Alfa-2a — used for decades with moderate results. Treatment is challenging and should be managed by a specialist hepatologist. | Dedicate subsection to HDV treatment. Mention bulevirtide as the major breakthrough. |
| 73 | Hepatitis D treatments | Hepatitis D | Same as above — plural variant for a broader treatment overview | Same intent as ‘hepatitis D treatment’. Cover all available and emerging options including bulevirtide and interferon. Note that treatment response rates vary and complete cure is difficult. | Use plural phrasing in one paragraph — it signals a comprehensive overview rather than a single drug focus. |
| 74 | Hepatitis D causes | Hepatitis D | Users want to know what causes Hepatitis D and who is at risk | Hepatitis D is caused by the Hepatitis D virus (HDV), a defective RNA virus that requires the HBV surface antigen (HBsAg) to replicate. It ONLY infects people already infected with Hepatitis B. Risk factors: IV drug use, unprotected sex with HBV/HDV-infected persons, blood transfusions. | Include in Hepatitis D overview. Emphasise the HBV co-dependency — unique biological concept. |
| 75 | D virus | Hepatitis D | Short search for the Hepatitis D / delta virus | ‘D virus’ refers to the Hepatitis Delta Virus (HDV). It is a unique satellite virus that cannot replicate without HBV. Vaccination against Hepatitis B indirectly prevents Hepatitis D as well. | Use ‘d virus’ naturally in the Hepatitis D section. Some users may find your article via this short search. |
| ◆ HEPATITIS E | |||||
| 76 | Hepatitis E treatment | Hepatitis E | Patients with Hepatitis E want to know treatment options | Most Hepatitis E cases resolve on their own within 4–6 weeks with rest, hydration, and avoiding alcohol and liver-toxic drugs. In immunocompromised patients (organ transplant recipients) or severe cases, Ribavirin may be used for 3–6 months. | Add to Hepatitis E section. Reassure readers that most cases self-resolve. |
| ◆ AUTOIMMUNE HEPATITIS | |||||
| 77 | Autoimmune hepatitis type 1 | Autoimmune Hepatitis | Patients diagnosed with AIH type 1 want to understand their specific condition | Autoimmune Hepatitis Type 1 is the most common form, characterized by positive ANA (antinuclear antibody) and/or anti-SMA (smooth muscle antibody). It primarily affects women. It can occur at any age. Responds well to corticosteroids (Prednisolone) and Azathioprine. | Add to Autoimmune Hepatitis section. Distinguish Type 1 from Type 2 (LKM-1 antibody positive, usually children). |
| 78 | Autoimmune hepatitis antibodies | Autoimmune Hepatitis | Patients want to understand which antibodies are tested for AIH | Key antibodies in Autoimmune Hepatitis: ANA (Antinuclear Antibody), ASMA (Anti-Smooth Muscle Antibody) for Type 1; Anti-LKM-1 (Liver Kidney Microsomal antibody) for Type 2; Anti-SLA (Soluble Liver Antigen) for a more severe subtype. | Add antibody table to AIH section. Helps readers understand their specific blood results. |
| 79 | Immune mediated hepatitis | Autoimmune Hepatitis | Medical or patient search for hepatitis caused by immune system dysfunction | Immune-mediated hepatitis includes autoimmune hepatitis (AIH) and drug-induced immune-mediated hepatitis (e.g., from checkpoint inhibitor cancer drugs like pembrolizumab). In both cases, the immune system attacks liver cells. | Use this term in the autoimmune section and also mention drug-induced immune hepatitis in a brief paragraph. |
| 80 | Life expectancy with autoimmune hepatitis | Autoimmune Hepatitis | Patients recently diagnosed with AIH searching for prognosis | With proper treatment, most people with Autoimmune Hepatitis have a normal or near-normal life expectancy. Studies show >80% achieve remission on Prednisolone + Azathioprine. Risk of cirrhosis is reduced significantly with adherence to treatment. Liver transplant is an option in refractory cases. | Address with reassurance. Many readers fear the worst at diagnosis. Empathy + evidence matters here. |
| ◆ GENERAL HEPATITIS | |||||
| 81 | Hepatitis is a disease of the | General Hepatitis | Students, patients, or curious readers wanting a basic definition | Hepatitis is a disease of the liver. The liver is the body’s largest internal organ, responsible for filtering blood, metabolising drugs, producing bile for digestion, and storing nutrients. When the liver is inflamed (hepatitis), all these functions are compromised. | Answer directly at the start of the article. Great for featured snippet optimisation. |
| 82 | Hepatitis is | General Hepatitis | Very basic search — want a simple definition | Hepatitis is inflammation of the liver. The word comes from Greek ‘hepar’ (liver) + ‘itis’ (inflammation). It can be caused by viruses, alcohol, autoimmune conditions, drugs, or toxins. | Use in the opening paragraph. Target featured snippet with a clear, concise one-sentence answer. |
| 83 | Hepatitis spread | General Hepatitis | General question about how any form of hepatitis spreads | Hepatitis spread varies by type. Hep A/E: contaminated food and water. Hep B/C/D: blood and body fluids. Hep B: also sexually and mother-to-child. Autoimmune and alcoholic hepatitis: not contagious. | Dedicate a clear ‘How Does Hepatitis Spread?’ section near article top. |
| 84 | Cholestatic hepatitis | General Hepatitis | Medical or patient search for a specific form of liver inflammation involving bile | Cholestatic hepatitis is a form of liver disease where bile flow is impaired (cholestasis) along with liver cell inflammation (hepatitis). It can be caused by viral hepatitis, drug reactions, pregnancy (intrahepatic cholestasis of pregnancy), or bile duct obstruction. Symptoms include severe itching, jaundice, and pale stools. | Add brief mention in ‘Other Types of Hepatitis’ section or a footnote. |
| 85 | Toxic hepatitis | General Hepatitis | Users want to know about hepatitis caused by chemicals, drugs, or toxins | Toxic hepatitis (also called drug-induced liver injury or DILI) is liver inflammation caused by exposure to toxic substances including medications (paracetamol overdose, antibiotics), herbal supplements, industrial chemicals, and recreational drugs. Stopping the offending substance is the primary treatment. | Add to ‘Causes of Hepatitis’ section. Many readers may be experiencing symptoms from herbal medicines. |
| 86 | Hepatitis rash | General Hepatitis | Patients experiencing skin symptoms want to know if it is hepatitis-related | Hepatitis can cause skin symptoms including jaundice (yellowing), itching (pruritus from bile salt accumulation), spider angiomas (tiny red blood vessels visible under skin), and palmar erythema (reddening of the palms). Hepatitis C specifically can cause lichen planus and purpura. | Include in Symptoms section. Add a note that skin symptoms are often early signs of liver disease. |
| 87 | Hepatitis is a disease of the | General Hepatitis | Duplicate search variation | (Covered above) — Hepatitis is a disease of the liver. Ensure this phrase appears naturally in the opening definition paragraph. | Target with a direct answer in the first 100 words of the article. |
| 88 | Liver in english | General Hepatitis | Non-native English speakers or students wanting to know the English word for liver | In English, the organ is called the ‘liver’ (جگر in Urdu/Hindi: ‘jigar’, yackrit in Sanskrit). It is the largest internal organ in the human body, weighing approximately 1.5 kg in adults. | Include in a beginner-friendly introduction paragraph. Helps reach multilingual audiences. |
| 89 | Hepatitis day | General Hepatitis | Users searching for World Hepatitis Day events or awareness campaigns | World Hepatitis Day is observed every year on 28 July. It was established by the World Health Organization (WHO) to raise awareness about viral hepatitis. The date marks the birthday of Nobel Prize-winning scientist Dr. Baruch Samuel Blumberg, who discovered the Hepatitis B virus. | Add a World Hepatitis Day section or callout box. Great for topical/seasonal content. |
| 90 | World hepatitis day | General Hepatitis | Same as hepatitis day — users want date, theme, and significance | World Hepatitis Day: 28 July each year. WHO theme changes annually (e.g., ‘One Life, One Liver’). The day promotes testing, vaccination, and treatment access globally. About 3,500 people die every day from viral hepatitis-related complications worldwide. | Great for topical SEO boost around July. Add a dedicated awareness section. |
| 91 | Chronic active hepatitis | General Hepatitis | Older medical term — users or doctors may encounter it in older records | Chronic active hepatitis is an older clinical term that was used before the hepatitis viruses were fully characterised. Today it is replaced by specific diagnoses like ‘chronic hepatitis B’, ‘chronic hepatitis C’, or ‘autoimmune hepatitis’. It referred to chronic liver inflammation with active necrosis. | Mention briefly as a historical/outdated term in a glossary or footnote. |
| 92 | Hepatitis is a disease of the | General Hepatitis | Variant | (Covered above) | (Already addressed) |
| ◆ LIVER DISEASE / OTHER | |||||
| 93 | VOD liver | Liver Disease / Other | Medical search for Veno-Occlusive Disease of the liver | VOD (Veno-Occlusive Disease), now called Sinusoidal Obstruction Syndrome (SOS), is a serious liver condition often seen after bone marrow/stem cell transplantation or exposure to certain herbal toxins (e.g., pyrrolizidine alkaloids). Not a form of hepatitis but affects liver function severely. | Add briefly in ‘Other Liver Conditions’ or ‘Complications’ section if targeting broad liver audience. |
| 94 | BCLC liver | Liver Disease / Other | Clinicians or informed patients searching for the BCLC staging system for liver cancer | BCLC (Barcelona Clinic Liver Cancer) is the most widely used staging system for hepatocellular carcinoma (HCC — liver cancer). It stages cancer from 0 (very early) to D (terminal) and recommends treatment at each stage. Relevant to hepatitis patients because chronic HBV and HCV are leading causes of HCC. | Mention in ‘Complications of Chronic Hepatitis’ section when discussing liver cancer risk. |
Disclaimer: Medical information provided is for educational and content-planning purposes only. Always verify clinical details with qualified healthcare professionals before publishing.
Also read: What is Dark Factory Industry 5.0 and COBOTS? (PPTX)
FAQ:
Is hepatitis curable?
Yes, in most cases. Hepatitis A and E resolve on their own. Hepatitis C is curable in over 95 percent of cases with modern DAA medications. Hepatitis B can be managed long-term and sometimes cleared. Hepatitis D is the hardest to cure but newer treatments like bulevirtide are showing promise.
Is hepatitis deadly?
Untreated chronic hepatitis B and C can lead to cirrhosis, liver failure, and liver cancer, which can be fatal. However, with early diagnosis and treatment, the risk is greatly reduced. Acute hepatitis E can be life-threatening for pregnant women.
Is hepatitis contagious?
All viral forms of hepatitis are contagious to some degree, but they spread in different ways. Hepatitis A and E spread through contaminated food and water. Hepatitis B, C, and D spread through blood and body fluids. None of the hepatitis viruses are spread through casual everyday contact like hugging or sharing cups.
What does hepatitis B surface antibody reactive mean?
It means your immune system has developed antibodies against the hepatitis B virus. This is a good result. It means you are immune, either from vaccination or because you have recovered from a past infection.
What does hepatitis B surface antigen reactive mean?
It means the hepatitis B virus is currently present in your blood. You are infected and could transmit the virus to others. You should see a doctor promptly for further evaluation and to discuss treatment options.
What is the difference between hepatitis B reactive and non reactive?
Hepatitis B reactive means a specific test came back positive and needs further investigation. Hepatitis B non reactive means no active infection or antibodies were detected for the marker being tested. These terms always need to be interpreted in context with your full hepatitis B panel by a qualified healthcare provider.
Conclusion: Knowledge is the First Step to Better Liver Health
Hepatitis is a broad term that covers a range of liver conditions with very different causes, presentations, and outcomes. From the highly curable hepatitis C, managed effectively today with medications like Harvoni, Epclusa, and Mavyret, to the more complex hepatitis B requiring long-term management and the emerging treatments for hepatitis D including bulevirtide, medical science has made remarkable strides.
Whether you are trying to understand a test result like hepatitis B surface antibody reactive, wondering if hepatitis is contagious, or looking for clear information on hepatitis symptoms, we hope this guide has provided the answers you were looking for.
If you suspect you may have hepatitis or have received a positive test result, do not delay. Speak with your healthcare provider as soon as possible. Early diagnosis and treatment save lives.
Disclaimer: This article is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.